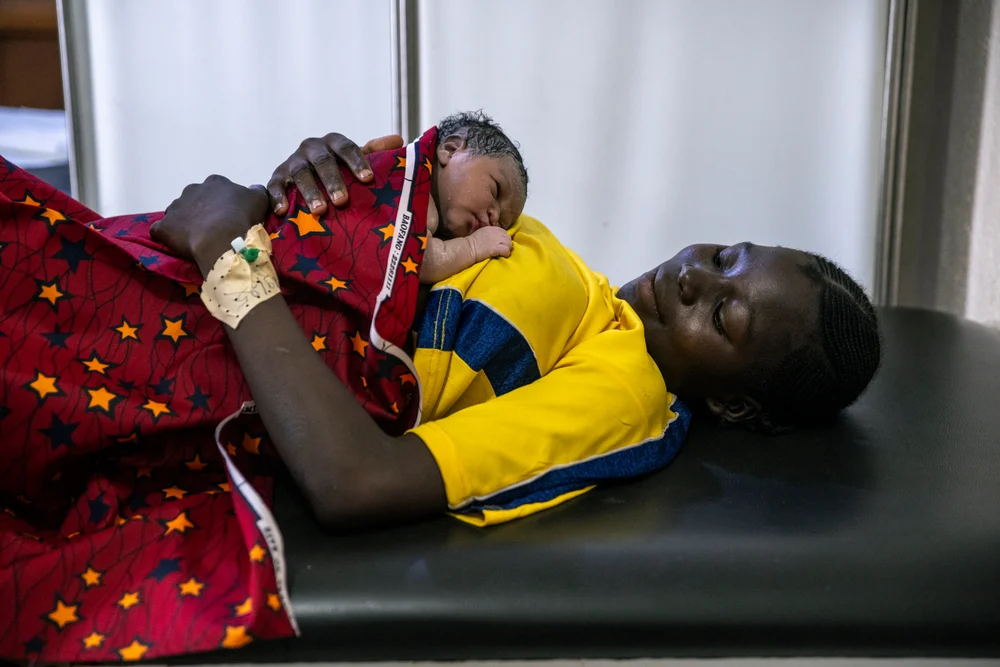
Maternal Mortality: Why Bringing New Life into the World Should Not End in Death
In many parts of the world, the moment that should mark the beginning of life is still shadowed by the risk of death. For healthcare professionals working in sexual and reproductive health, this reality is neither abstract nor distant, but part of a daily struggle to close the gap between what medicine can achieve and what health systems actually deliver. A powerful reflection of this gap is captured in a Médecins Sans Frontières (MSF) account, available here: https://msf.org.au/article/stories-patients-staff/maternal-mortality-bringing-new-life-world-shouldnt-end-death, where the experiences of patients and providers reveal how preventable maternal deaths continue to persist in fragile settings.
Every day, hundreds of women die from complications related to pregnancy and childbirth, and the vast majority of these deaths occur in contexts where access to timely, skilled medical care is limited or absent. These are not rare or unpredictable tragedies, but outcomes linked to well-known and treatable conditions such as hemorrhage, sepsis, hypertensive disorders, obstructed labour, and complications from unsafe abortion. What transforms these complications into fatal outcomes is not their severity alone, but the absence of functioning systems capable of responding in time.
The stories shared by MSF highlight a recurring pattern that transcends geography. Women often face multiple, compounding delays, beginning with the decision to seek care, followed by the challenge of reaching a facility, and finally the uncertainty of receiving appropriate treatment once they arrive. In humanitarian settings, these delays are amplified by conflict, displacement, and the collapse of health infrastructure, leaving pregnant women among the most vulnerable populations.
Yet within these constraints, the presence of trained healthcare professionals and even basic emergency obstetric care can mean the difference between life and death. MSF’s experience demonstrates that when women have access to skilled staff, essential medications, and surgical capacity, the majority of life-threatening complications can be effectively managed. This underscores a fundamental truth for clinical practice: maternal mortality is not simply a reflection of biological risk, but of systemic failure to provide timely and adequate care.
At the same time, maternal health cannot be separated from the broader continuum of reproductive healthcare. Antenatal care, family planning, safe abortion services, and postnatal follow-up all contribute to reducing risk and improving outcomes. Where these services are fragmented or inaccessible, the burden of complications increases, often culminating in emergencies that could have been prevented.
For healthcare professionals, these realities reinforce the importance of both clinical competence and system-level engagement. Saving lives in obstetric care depends not only on individual skill, but on the existence of referral pathways, functional facilities, and policies that prioritize access and equity. The MSF narrative ultimately reframes maternal mortality as an avoidable outcome, one that persists not because solutions are unknown, but because they remain unevenly implemented.
In this light, the act of giving life should never carry the expectation of loss. The challenge for modern healthcare systems is not only to reduce maternal mortality, but to ensure that safe, respectful, and timely care becomes the standard rather than the exception.




















